Scientists say the bacteria behind the Black Death still circulates — and outbreaks still happen today.

It was one of the deadliest diseases in human history, killing tens of millions during the Middle Ages. But the plague never truly vanished. The same bacteria that caused the Black Death still survives in wild rodent populations around the world, occasionally infecting humans. Though modern medicine makes large-scale outbreaks far less likely, experts say changing climates, human encroachment, and antibiotic resistance could make conditions ripe for its return — in ways few expect.
1. The Plague Bacterium Still Exists in Nature
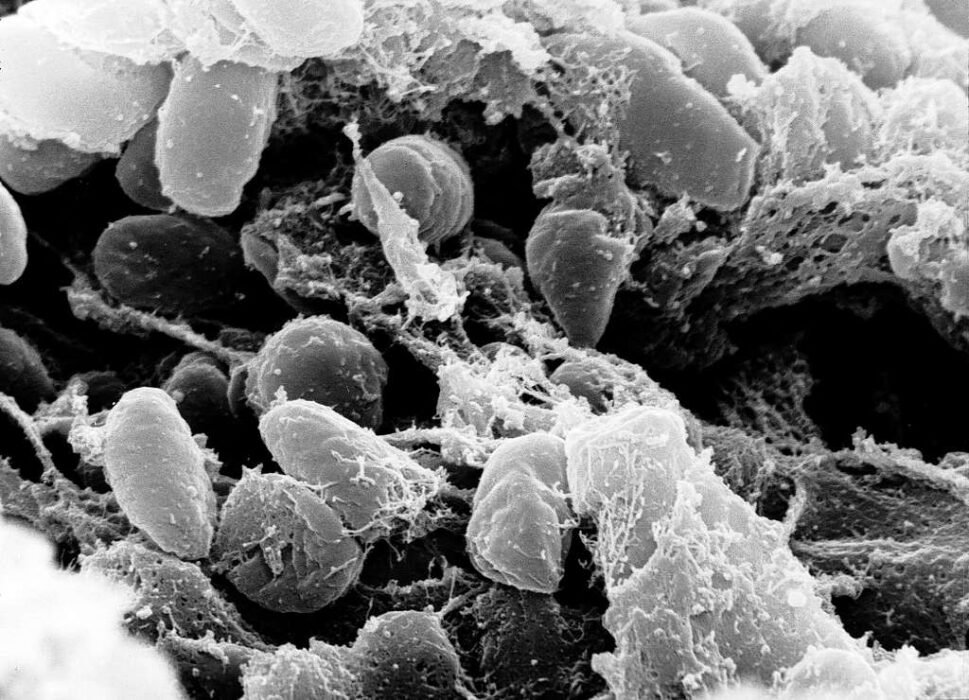
The plague is caused by Yersinia pestis, a bacterium that continues to survive in the wild. It circulates through small mammals and fleas in what scientists call “plague reservoirs,” which exist in regions of Africa, Asia, and even the western United States. These natural ecosystems allow the bacteria to persist indefinitely, usually without drawing much attention.
Researchers have identified plague reservoirs in places like Madagascar, Mongolia, and the American Southwest. These pockets of infection are carefully monitored because, while rare, transmission to humans can still occur when people come into contact with infected animals or their fleas.
2. Modern Outbreaks Still Occur Every Year
Despite its historical reputation, the plague hasn’t disappeared — it continues to infect people every year. The World Health Organization reports between 200 and 500 human cases globally on average, mostly in rural regions with limited sanitation and high exposure to rodents.
Recent outbreaks have occurred in Madagascar, the Democratic Republic of Congo, and Peru. Thanks to antibiotics and better surveillance, deaths are far less common today, but these recurring cases serve as a reminder that the bacterium never left the planet.
3. How the Plague Spreads Between Animals and People

Transmission still occurs primarily through fleas that have fed on infected rodents. Humans can become infected if bitten by those fleas, or by handling sick or dead animals carrying Yersinia pestis. Rarely, if the bacteria reach the lungs, it can spread between people via airborne droplets — a form known as pneumonic plague.
Because of these multiple transmission routes, public health agencies maintain ongoing surveillance of rodent populations in plague-prone areas. Early detection in animals is often the best way to prevent human exposure before outbreaks occur.
4. The Role of Climate and Ecosystem Change

Environmental conditions can strongly influence how and where plague spreads. Shifts in temperature, rainfall, and drought cycles affect the populations of rodents and fleas, potentially driving them closer to human settlements. Scientists have found that warmer, wetter conditions can temporarily increase flea survival rates, raising the risk of transmission.
In places like Central Asia and the American West, plague activity often spikes following ecological disruption or rapid climate swings. As climate change accelerates, experts warn that these outbreaks could become more frequent or appear in unexpected regions.
5. Madagascar Has Seen Some of the Worst Modern Outbreaks

Madagascar remains one of the world’s most active plague hotspots. Outbreaks occur almost every year, particularly between September and April. Most cases are bubonic, but in 2017, a severe epidemic involving pneumonic plague infected over 2,000 people and killed more than 200.
Poor sanitation, urban crowding, and close contact with rodents helped the disease spread rapidly. Following that crisis, the country expanded surveillance networks and medical response teams, but the persistence of plague in Madagascar shows how environmental and economic factors can still enable deadly flare-ups.
6. Antibiotics Work — But Resistance Is a Growing Concern

Modern antibiotics make plague highly treatable when detected early. Drugs such as streptomycin, doxycycline, and ciprofloxacin can cure most infections within days. With quick treatment, recovery rates exceed 90 percent, making widespread pandemics unlikely under current conditions.
However, researchers have found signs of antibiotic resistance in a few Yersinia pestis strains. Though rare, these mutations could pose future challenges if they spread in areas with limited healthcare access. Continuous monitoring and strong global reporting systems remain essential to keep treatments effective.
7. The Pneumonic Form Is the Most Dangerous

The plague appears in three forms: bubonic (affecting lymph nodes), septicemic (infecting the bloodstream), and pneumonic (targeting the lungs). Of these, pneumonic plague is the most contagious and deadly if untreated. It spreads through respiratory droplets when an infected person coughs or sneezes.
Pneumonic cases progress rapidly — sometimes within 24 hours — and require immediate antibiotic treatment. Although outbreaks are rare today, health agencies consider this version of the disease a serious threat in overcrowded environments or regions with weak healthcare systems.
8. Wildlife Surveillance Is Key to Prevention

Because Yersinia pestis persists naturally among wild animals, monitoring those populations is critical for early warning. Wildlife biologists routinely test rodents, fleas, and other species in known reservoir zones. Detecting the bacteria in animals often gives public health officials time to warn nearby communities.
These programs have proven successful in preventing human infections. In parts of the U.S. and Asia, targeted rodent control and flea management have kept outbreaks small and contained — a model for global prevention efforts.
9. Climate Change Could Expand Plague Zones

Warming temperatures and ecosystem disruption could allow plague-carrying fleas and rodents to expand their range. Some models predict that higher altitudes and northern regions may become more suitable for Yersinia pestis reservoirs over time.
This expansion would not necessarily trigger major outbreaks, but it could increase sporadic infections in areas previously considered low risk. Scientists emphasize that climate change doesn’t create new diseases — it changes the conditions that allow old ones to persist and spread.
10. Urbanization Raises the Risk of Contact

As human populations grow and expand into previously wild areas, encounters with rodents and their fleas become more frequent. Construction, deforestation, and agricultural development can all disrupt natural habitats and push infected wildlife into closer contact with people.
This increased interaction elevates the potential for zoonotic diseases like plague to jump species barriers. Experts argue that responsible land management and sanitation practices are essential in keeping such risks low, especially in developing regions.
11. Outbreaks Could Spread Faster in a Globalized World

While medical advances make plague easier to treat, modern travel could accelerate its spread before detection. Infected individuals can move across regions or borders within hours, potentially exposing new populations before symptoms appear.
Public health systems now use digital surveillance and rapid testing to prevent global spread. The World Health Organization maintains alert networks to track suspected cases in real time — tools that didn’t exist in previous centuries.
12. Scientists Say Awareness Is the Best Defense

Experts agree that the risk of another medieval-scale pandemic is extremely low, but awareness is still essential. Recognizing plague as a living disease — not just a historical relic — helps ensure rapid response and public readiness.
With strong healthcare systems, early diagnosis, and continued investment in surveillance, outbreaks can remain rare and contained. The lesson from scientists is clear: humanity already has the tools to control the plague — but only if it stays alert.
