New research suggests fragments of the virus can linger, group together, and damage immune defenses long after infection.
For many people, COVID-19 doesn’t fully end when the virus leaves the body. Scientists are increasingly finding evidence that remnants of the virus can persist and continue interacting with the immune system in unexpected ways.
Recent laboratory research shows that pieces of the coronavirus may band together and actively kill key immune cells. These findings offer a possible explanation for lingering immune problems and some of the symptoms reported by people with long COVID.
1. The virus may leave behind more than memories

After an infection clears, viral particles are usually broken down and removed. In this case, researchers found that fragments of the coronavirus can remain in the body.
These remnants are not complete viruses, but they are not harmless debris either. Their persistence suggests COVID-19 may have longer-lasting biological effects than originally assumed. This challenges the idea that recovery always means a clean reset.
2. The fragments are pieces of viral proteins
The lingering material consists of broken protein fragments from the virus. These pieces cannot infect cells or replicate on their own.
However, they still retain biological activity. Scientists found that these fragments can interact with immune cells in damaging ways. This makes them more than just inactive leftovers.
3. The fragments can group together
Instead of acting alone, the viral remnants appear to cluster. Researchers observed that these protein fragments can join into larger complexes.
Working together, they become more potent than individual fragments. This group behavior allows them to overwhelm immune cells more effectively. The researchers compared this behavior to hunting in packs.
4. Key immune cells are the main targets
The study focused on T cells, which play a critical role in fighting infections and coordinating immune responses. These cells are essential for long-term immunity.
When exposed to clustered viral fragments, T cells began to die. Losing these cells weakens the immune system. This loss could leave the body more vulnerable even after the original infection ends.
5. The damage happens without live virus

One of the most surprising findings was that no active virus was needed. The immune cells were harmed even in the absence of viral replication.
This suggests the body doesn’t need to be reinfected for damage to continue. Viral debris alone may be enough to trigger immune cell death. That shifts how scientists think about post-infection effects.
6. The process resembles immune sabotage
Normally, the immune system clears viral debris without issue. In this case, the fragments appear to turn the system against itself.
By killing off immune cells, the remnants may interfere with recovery. This kind of internal sabotage could explain prolonged immune dysfunction. It also helps explain why some people struggle to bounce back.
7. The findings may help explain long COVID

Many people with long COVID report fatigue, brain fog, and frequent illness. These symptoms are consistent with a weakened or disrupted immune system.
If immune cells are being destroyed long after infection, it could account for those experiences. The study provides a biological mechanism that links lingering viral material to lasting symptoms. This connection has been difficult to prove until now.
8. Not everyone may be affected the same way

Researchers believe individual immune responses play a role. Some people may clear viral fragments quickly, while others may not.
Genetics, severity of the original infection, and immune health could all influence outcomes. This helps explain why long COVID affects some people more than others. The variability has been one of the biggest puzzles.
9. The discovery changes how recovery is viewed
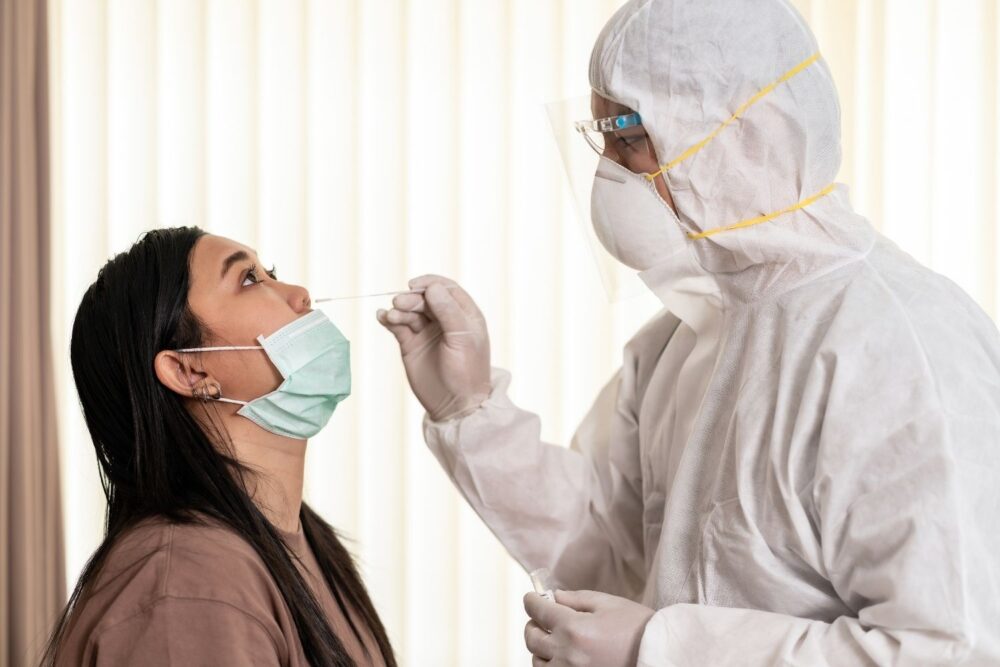
Recovery is often measured by negative tests and reduced symptoms. This research suggests recovery may be more complex at the cellular level.
Even when someone feels better, immune damage may still be occurring. This could affect how doctors monitor and treat post-COVID patients. Long-term follow-up may be more important than previously thought.
10. The findings could influence future treatments
Understanding how viral fragments harm immune cells opens new research paths. Scientists may be able to develop therapies that help clear these remnants.
Targeting the fragments directly could protect immune cells from further damage. This approach would differ from traditional antiviral treatments. It focuses on cleanup rather than infection control.
11. COVID-19 may leave a longer biological footprint

The study adds to growing evidence that COVID-19 can have lasting effects beyond acute illness. Viral remnants may continue interacting with the body long after symptoms fade.
Rather than being a short-term infection for everyone, COVID-19 may alter immune systems in subtle but meaningful ways. These insights are reshaping how scientists understand both recovery and long-term risk.
